Many individuals with Irritable Bowel Syndrome (IBS) would be willing to sacrifice 10 to 15 years of life expectancy for an immediate cure for their condition.
A study involving nearly 2,000 people with IBS revealed this sentiment.1
In another study, individuals with IBS expressed a willingness to take a medication with a one percent risk of sudden death if it meant their symptoms would be cured2. These symptoms can include urgent episodes of diarrhea, gas, or persistent constipation.
Some individuals with IBS endure abdominal pain during flare-ups that they describe as more severe than childbirth. These episodes can impact concentration, disrupt sleep, and hinder work productivity.3
As a result, many individuals with IBS organize their lives around access to private, clean restrooms. The fear of sudden flare-ups causes some to avoid restaurants, social gatherings, and even public exercise.
This pervasive worry is known as gastrointestinal-specific anxiety and can affect various aspects of life, from social relationships to overall well-being. It is also the primary reason why individuals with IBS report a lower quality of life compared to those with other chronic conditions like heart disease, diabetes, and end-stage kidney disease.4
If you or someone you know has IBS, there are strategies to manage the condition.
Precision Nutrition Super Coach Sarah Maughan, certified through Monash University, a global leader in understanding the connection between food sensitivities and IBS, has witnessed how lifestyle changes can prevent flare-ups, reduce GI anxiety, and enable individuals with IBS to lead fulfilling lives.
“I hope that everyone with IBS realizes they have options, whether that involves consulting a healthcare provider for medication and/or working with a health coach to learn about lifestyle modifications and how to implement them,” says Maughan.
In this article, we will delve deeper into Maughan’s insights. You will also discover:
-
- What IBS entails, including why it occurs and the various ways it can manifest
-
- What bowel movements can indicate about digestive tract health
-
- Five evidence-based lifestyle changes that can alleviate IBS symptoms
-
- The most effective approach to determine which foods trigger IBS symptoms for you or someone you know (and which foods are generally safe to consume)
Additionally, if you are a health coach, you will learn how to assist clients with IBS while staying within your professional scope.
Understanding Irritable Bowel Syndrome (IBS)
Commonly referred to as “spastic colon,” IBS is the most frequently diagnosed digestive disorder globally, affecting approximately 14% of adults.5
Unlike conditions like Crohn’s disease and other inflammatory bowel diseases (IBD), IBS does not result in structural changes to the gut. Diagnostic imaging by healthcare professionals does not reveal infections, inflammation, bowel wall damage, or other signs of disease.
Previously, the absence of visible disease led many healthcare professionals to believe that IBS was primarily psychological. However, this perspective has evolved in recent years.
Experts now regard IBS as a functional neuro-gastrointestinal disorder.
This indicates that there is suboptimal communication between the nerves in the GI tract and the brain, resulting in the brain transmitting unnecessary pain signals and disrupting normal bowel function.
Common Symptoms of IBS
Symptoms of IBS can be intermittent, with some individuals experiencing periods of relief lasting months or years, only to encounter severe flare-ups that can persist for hours to weeks.
Moreover, not all individuals with IBS exhibit the same range of symptoms, which can complicate the diagnostic process.
The diagram below depicts the spectrum of IBS symptoms.

Factors Contributing to IBS
Researchers are still exploring the reasons behind altered gut function in individuals with IBS. However, several theories have emerged.
One hypothesis suggests that nerve endings in the GI tract may be overly sensitive in individuals with IBS. This sensitivity can manifest in two distinct sets of symptoms.
▶ Hypersensitive nerves transmit pain signals to the brain, leading individuals with IBS to notice digestive processes that others may not perceive. For instance, small gas bubbles could be highly discomforting for someone with IBS but not bothersome for someone without the condition.
▶ Overactive nerves can prompt excessive contractions of GI muscles, resulting in gas, bloating, and diarrhea. Conversely, if these nerves underreact, the muscles may not contract forcefully enough, slowing down food passage through the intestine and causing constipation.
Another theory implicates disturbances in the gut microbiome, offering an explanation for why some individuals develop IBS symptoms after experiencing a severe GI illness like Norovirus.
Diagnosing IBS
If you suspect IBS in yourself or a client, it is advisable to consult a qualified healthcare professional.
IBS symptoms overlap with various other gastrointestinal conditions and health issues that may necessitate medication, surgery, or medically supervised lifestyle changes. These conditions include infections, inflammatory bowel diseases, celiac disease, cancer, and food allergies, among others.
It is crucial to seek medical attention if you or your client experience any of the following:
-
- Rapid, unintentional weight loss
-
- Rectal bleeding, blood in stools, or vomiting blood
-
- Episodes of disruptive diarrhea during sleep
-
- Diarrhea accompanied by fever
-
- Continuous abdominal pain
-
- Sudden onset of GI symptoms after age 50
Types of IBS
In addition to ruling out other GI conditions, healthcare professionals will inquire about specific symptoms to determine the type of IBS affecting you or your client:
-
- IBS-D, characterized by predominant diarrhea
-
- IBS-C, marked by constipation
-
- IBS-M, involving alternating bouts of diarrhea and constipation
-
- IBS-U, indicating symptoms that do not neatly fit into any of the above categories
Your or your client’s IBS type will inform the recommended course of action by the healthcare professional.
For IBS-D, a healthcare provider might suggest a brief course of antibiotics and antidiarrheal medication. Conversely, for IBS-C, they may recommend a fiber supplement, non-habit-forming laxative, or other medications to alleviate pain perception and regulate bowel movements.
Preparing for a Medical Consultation: Pre-Appointment Checklist
To maximize the effectiveness of the visit, it is helpful to prepare responses to the following questions in advance:
-
- Duration of symptoms
-
- Changes coinciding with symptom onset (e.g., changes in stress levels, dietary habits, recent travel)
-
- Prior incidents of food poisoning or gastroenteritis
-
- Dietary fiber intake
-
- Sleep quality and duration
-
- Physical activity frequency
Additionally, consider:
Observing Bowel Movements
Maintaining a fecal diary for a few weeks before the appointment can be beneficial.
Record bowel movement frequency and other symptoms, utilizing the Bristol Stool Chart to assess stool quality. This information aids healthcare professionals in diagnosing IBS and determining the specific type.

(For further insights on interpreting stool characteristics, refer to: 6 reasons you should prioritize bowel health)
Strategies for Managing IBS: 5 Approaches to Support Gut Health and Function
In recent years, the FDA has approved several new prescription medications for IBS, along with a medical device that stimulates cranial nerves behind the ear.
Furthermore, numerous research studies have explored the correlation between IBS and various lifestyle practices, yielding promising results.
Here are five evidence-based methods to alleviate IBS symptoms (many of which also promote overall health):
IBS Relief Strategy #1: Incorporate Physical Activity
Regular exercise has been linked to reduced symptom severity and flare-ups in individuals with IBS compared to sedentary counterparts.
For instance, a study found that individuals with IBS who engaged in moderate walking for an hour three times per week experienced significant relief from bloating and abdominal pain within 12 weeks.6
The precise mechanisms through which exercise benefits IBS are not fully understood.
According to some studies, exercise may mitigate stress, enhance mental well-being, and foster improved communication between the gut and the brain.7 8
Alternatively, exercise might promote the proliferation of beneficial gut bacteria, aiding in more efficient food breakdown and reduced inflammation.9
IBS Relief Strategy #2: Stress Management
Anxiety, stress, and depression can trigger stress hormones like norepinephrine and cortisol, which may:
-
- Heighten gut-related pain signals
-
- Disrupt the equilibrium of gut bacteria (microbiome)
-
- Augment intestinal permeability, potentially allowing harmful substances into the bloodstream10 11 12
Coping with stress is not a simple task.
Mere directives to “stop stressing out!” are unlikely to be effective and might even exacerbate stress levels.
Therefore, Precision Nutrition-certified coaches like Maughan guide clients in focusing on manageable aspects, such as cultivating self-compassion or experimenting with stress-reducing techniques like yoga, breathing exercises, or leisurely walks.
As depicted in the image below, clients can influence how they perceive, respond to, and anticipate stressors, albeit not always the stressors themselves.
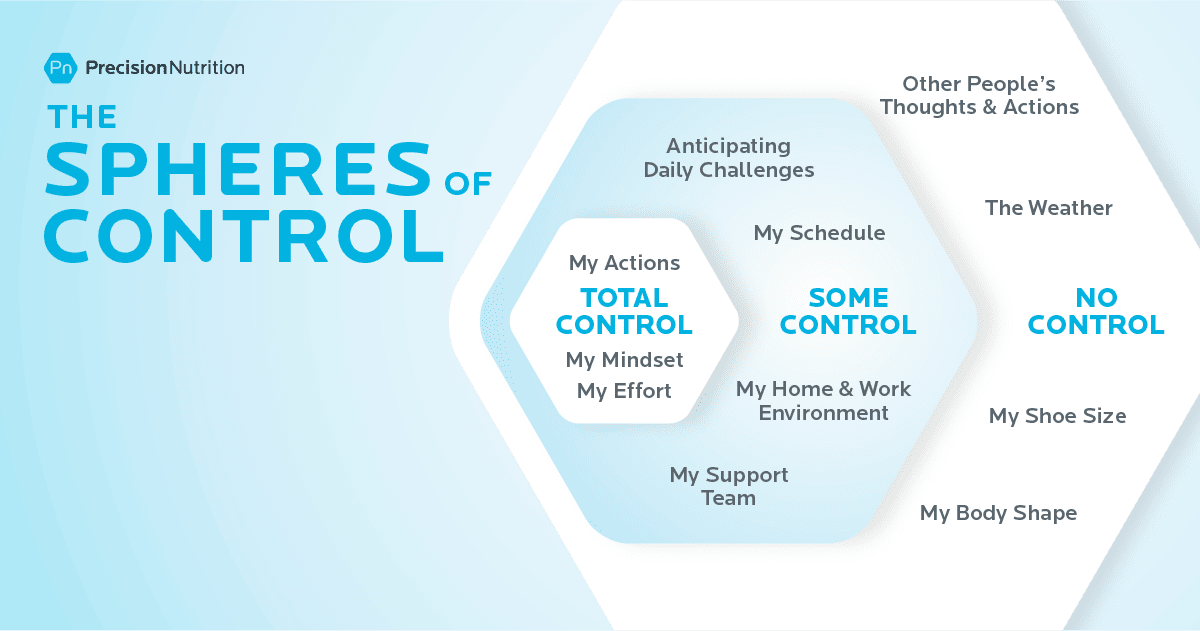
Encouraging clients to focus on aspects within their control often cultivates a sense of calmness and efficacy.
(For assistance in helping clients discern controllable versus uncontrollable factors, utilize our complimentary worksheet: Sphere of Control Worksheet)
(Assess your current stress load by taking our complimentary quiz: Do you have a Stress Bod?)
IBS Relief Strategy #3: Pace Your Eating
Precision Nutrition coaches advocate for slower, more relaxed eating habits.
Although slow eating aids in consuming fewer calories, it also tends to alleviate or eliminate GI issues like acid reflux, bloating, and pain.
Slower eating often entails increased chewing. In addition to mechanically breaking down food, heightened chewing permits oral digestive enzymes to initiate food breakdown. Consequently, the stomach and intestines encounter reduced strain.
Moreover, eating in a relaxed environment tends to lower stress hormone levels like norepinephrine and cortisol, diminishing the likelihood of heightened pain signals.
Maughan highlights the significance of this practice for parents, acknowledging the challenges of undistracted, peaceful eating while caring for young children.
(Although seemingly simple, slow eating is more demanding than commonly perceived and significantly impactful. Learn more: Embark on the slow-eating 30-day challenge.)
IBS Relief Strategy #4: Address Sleep Concerns
Research indicates that individuals with IBS often experience shallow, less restorative, and interrupted sleep.13
Despite sleeping longer hours overall than those without IBS, individuals with the condition frequently report feeling less rested.
This fatigue can initiate a detrimental cycle. Unrefreshing sleep typically elevates stress hormone levels, exacerbating gut pain.14
Furthermore, sleep-deprived individuals tend to experience heightened daytime hunger, particularly for fatty and sugary foods, prompting consumption of items likely to trigger IBS symptoms—and often in haste.
Halting this cycle poses a challenge.
Similar to stress management, individuals cannot simply compel themselves to sleep more restfully.
Nevertheless, the first three strategies—exercise, stress reduction, and slower eating—can collectively contribute to improved sleep quality.
Some Precision Nutrition clients have found that consuming a smaller, earlier dinner allows for better digestion prior to sleep. Others report that engaging in a calming pre-bed routine, such as foam rolling, guided meditation, a bath, or journaling, proves beneficial.
(Access optimal sleep practices by perusing our infographic: The power of sleep)
IBS Relief Strategy #5: Evaluate Dietary Choices
While there is no universal IBS diet, experts have identified several food categories that tend to provoke symptoms in many individuals. These include:
▶ Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols (FODMAPs), a group of carbohydrate-rich foods poorly absorbed in the small intestine. Even in individuals without IBS, these foods typically decelerate digestion and attract moisture. When gut bacteria ferment them, gas is produced, stretching the intestinal wall. While most individuals experience inconspicuous digestion slowing and gas production, individuals with IBS may endure intense discomfort. High-FODMAP foods comprise wheat, rye, barley, onions, garlic, beans, dairy, honey, cashews, certain processed meats, and numerous fruits and vegetables. (Further insights on FODMAPs are detailed in the subsequent section.)
▶ Caffeinated beverages and foods, particularly coffee, can stimulate stress hormone release, augment stomach acid secretion, enhance colon muscle contractions, and irritate intestinal linings.15
▶ Alcoholic beverages and spicy foods may irritate the gut.16 17
▶ High fructose corn syrup and sugar alcohols like sorbitol and mannitol have been associated with gas, bloating, and diarrhea in susceptible individuals.18 19
▶ Fatty, greasy foods can impede digestion, attract moisture, resulting in loose stools, bloating, and gas.20 21
While the notion of forgoing foods and beverages on the aforementioned list may be daunting, it is crucial to recognize that:
Not all individuals with IBS react to the same foods and beverages.
“Each person may have different triggers,” notes Maughan. “Hence, it is imperative to discern what makes your body feel optimal and what doesn’t.”
For instance, apples may be problematic for some but well-tolerated by others. Similarly, one may thrive on green tea but struggle with black tea. An individual might handle a modest beer serving but not a full pint. While a gluten-free diet may suit certain individuals, others may not benefit from it.
Many individuals find relief by avoiding specific high-FODMAP foods. Nevertheless, you might only be sensitive to select FODMAPs. In such cases, eliminating all FODMAPs might prove overly restrictive and challenging to sustain consistently.
Thus, undertaking an elimination diet to pinpoint troublesome foods and beverages—and discerning the quantities that can be safely consumed—can be advantageous, Maughan recommends. Further details on elimination diets will be explored in the subsequent section.

